Pilonidal disease has progressed from a condition that would require surgical excisions with the usual scope to one that currently has multiple viable solutions. If you’ve been studying treatment options, you won’t be surprised to see how many more modern pilonidal cyst treatments aim for speedier healing, less pain and lower recurrence rates. So some of the strategies in the new era can help you decide on your care and to not use the past that had taken some time to recover too.
What are the Minimally Invasive Pilonidal Treatments?
They tend to be non-invasive — focused on the cyst or the sinus tract, with little or no surgery to remove the surrounding tissue. Rather than widespread surgical removal, approaches such as these involve clearing debris (debris removal), destroying the lining of the cyst and promoting its natural healing. Pilonidal disease is a condition in which hair as well as debris gets lodged in the skin, forming a pocket that can fill with fluid and become infected. Conventional surgery will often clear much of this area entirely, while minimally invasive methodologies target the underlying disease and maintain normal tissue. Newer strategies are particularly attractive for reducing trauma to the body and facilitating a faster return to activities of daily living
How does your Laser Pilonidal Treatment Work?
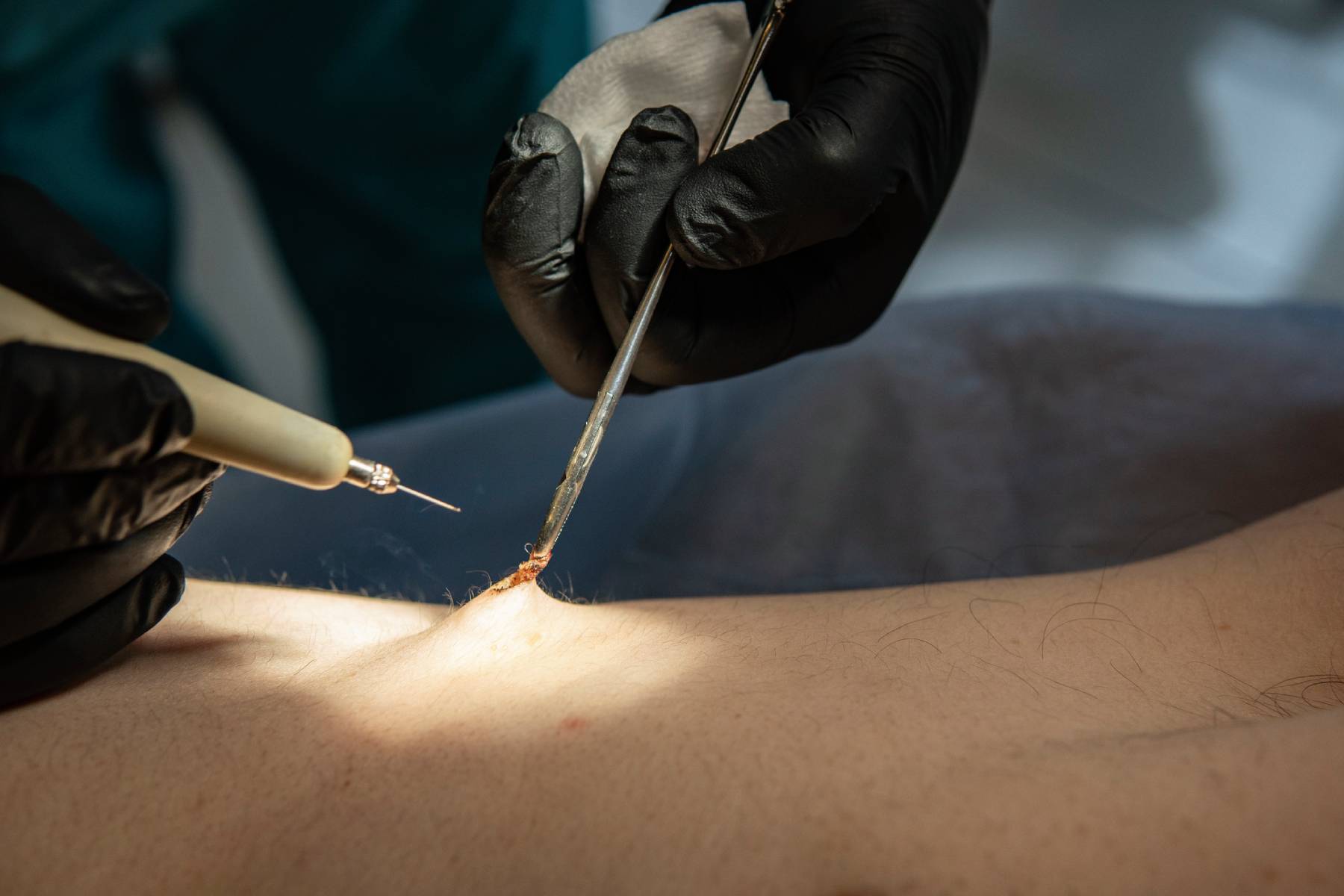
The most developed treatment now is laser pilonidal (also known as laser pilonidal plasty). This technique targets light energy to kill the cyst lining and close the sinus tract from the inside. It involves cleaning and removing hair and debris from the area before the procedure. In the sinus tract, a small laser probe is inserted with precise energy to remove infected tissues and seal it. Because the procedure is minimally invasive, there is no large open wound. This greatly diminishes pain, significantly reduces the chance of complications and shortens recovery time. Many patients return to normal activities much sooner when compared to traditional surgery.
What is Phenol Treatment and Why Does It Work?
Phenol treatment is another minimally invasive option which has been recognized in this same last decade. It consists of putting a chemical solution into the cyst cavity under the aegis of this test results in destruction of lining and promotion of healing. Phenol acts as a cauterizing agent and it has controlled inflammatory activity which aims to clear cysts by closing the tract. This procedure is standard in an office and does not require major surgery. Experience on the clinic has shown that phenol treatment can be extremely successful, with numerous patients resolving after few sessions. Use is especially beneficial for people with mild disease or early disease and when people are not seeking invasive treatment.
Are Flap Surgeries Yet to Occur Yet?
Where less invasive options are becoming more and more accepted, flap procedures remain beneficial for the treatment of severe or recurring cases. Approaches such as the rhomboid flap and Karydakis flap are also used which are techniques in which you take out the affected tissue and then rebuilding the whole area with other skin as the surface. These are procedures in order to flattening the gap between the buttocks, before more hair and other debris can build up again. Flap surgery that targets the underlying anatomy can help greatly reduce recurrence risk by improving the patient’s overall recovery. More invasive than those therapies involving laser or phenol, modern flap procedures are far more elegant than their predecessor surgical procedures and result in prolonged, long-term outcomes for patients suffering with severe disease.
What About Conventional Excision Surgery?
Traditional excision, whereby the cyst and surrounding tissue are pulled out, remains a common technique, although newer methods have made it far less common. This can be either leaving it open for healing or sewing the wound shut aseptically. Efficient as this approach is, excision is often associated with longer healing times and a greater risk of complications than minimally invasive options. Open wounds sometimes need to be cared for for weeks and they might need to be dressed and cured, and recovering can be more stressful. As a result, many of them will now just let treatment continue with regular excision for severe/comorbid patients when other therapies do not help.
How Do Caregivers Select Appropriate Care?
The most effective path of treatment for chronic pilonidal disease varies depending on several dimensions: its severity, whether it is acute or chronic, and whether it has recurred. When an infected abscess is first indicated, the surgeon may decide that the opening and pilonidal cyst drainage are necessary to ease discomfort and decrease inflammation. For chronic or recurring disease, the objective is to remove sinus tract and prevent recurring infections. Minimal invasive techniques are usually favoured when possible, and more invasive procedures are reserved for more advanced cases. A specialist will assess the size and depth of the cyst and the presence of multiple tracts — then make decisions on a treatment plan based on that information. Such a personalized method brings the best possible outcome.
Why are Modern Therapies Changing the Standard of Care?
The move to minimally invasive pilonidal cyst treatment is indicative of a larger shift in medicine toward the idea of giving patients control over their lives. Techniques focus less on aggressive removal than on effectiveness, comfort, and quality of life in the present. Techniques such as laser therapy and phenol treatment also reduce postoperative pain and speed recovery over time along with the ease of returning to work or activities of daily living. Simultaneously, sophisticated surgical techniques such as flap procedures target underlying causes of recurrence to improve long-term success rates. The ways in which patients and providers respond to pilonidal disease are evolving through these innovations. Treatment for this illness is now possible to provide and less intimidating than it’s ever been.
Conclusion
Pilonidal disease doesn’t still need to equate to extended recovery times or invasive surgery being the only option anymore. Patients benefit from a plethora of pilonidal abscess treatment options available to them, ranging from laser therapy and phenol treatment to sophisticated surgical techniques for more advanced cases, thanks to advancements in medical treatment of pilonidal cysts. Both strategies have their advantages, and the choice is highly influenced by a person’s current state and aspirations. The way I see it — with knowledge of these options you can plan treatment in the direction of these options based on effective treatment choices along with a more efficient process of recovery that can be guided by their expert.