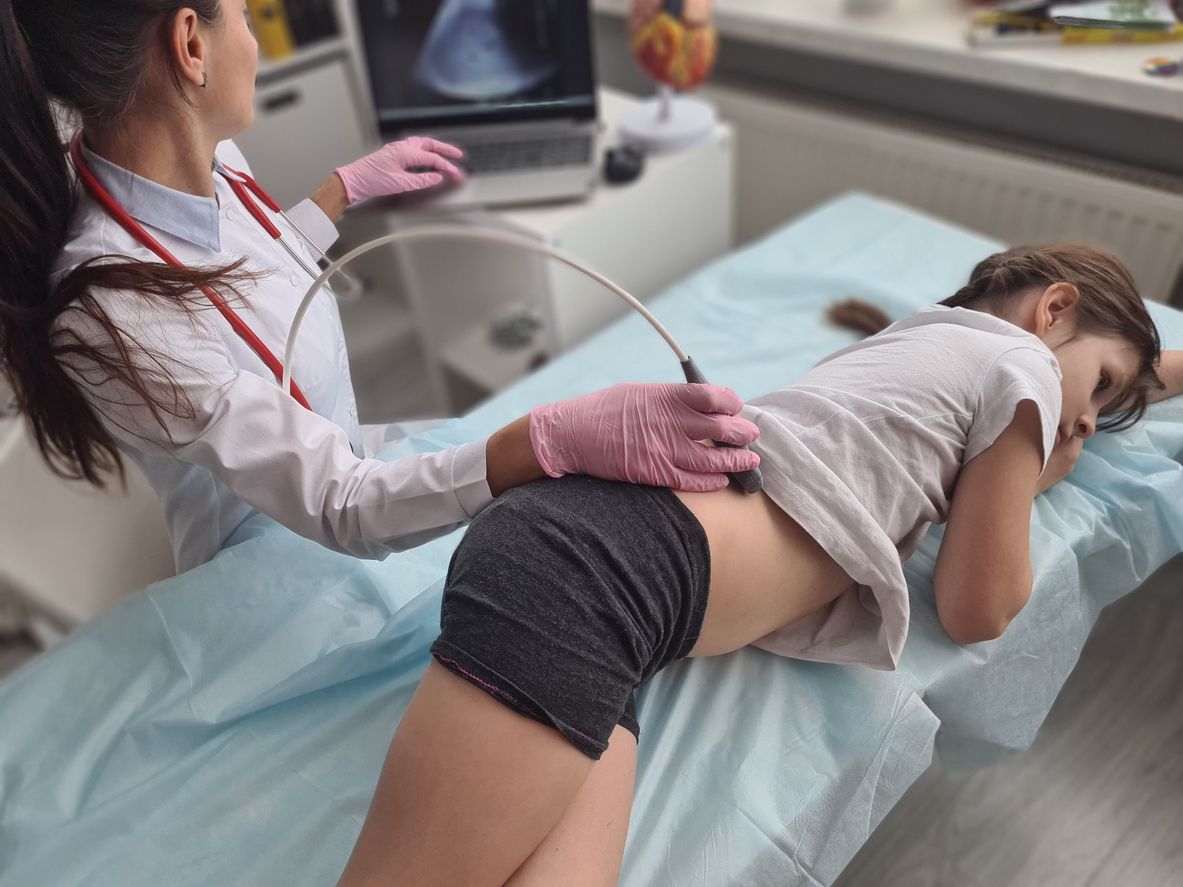
Pilonidal disease is a skin condition characterized by the formation of a cyst or sinus tract near the tailbone. This condition is often painful and uncomfortable, necessitating medical attention. This article will delve into the specifics of pilonidal disease, investigating its symptoms, causes, and treatment options, with a particular emphasis on pilonidal sinus surgery and the management of a pilonidal cyst infection.
Overview of Pilonidal Disease:
Pilonidal disease refers to the development of a cyst or sinus tract in the cleft of the buttocks, just above the tailbone. The term “pilonidal” is derived from Latin and means “nest of hairs,” alluding to the condition’s underlying cause. The cyst or sinus forms when hair follicles become blocked and infected, causing debris and bacteria to accumulate.
Symptoms of Pilonidal Disease:
Pilonidal disease causes a variety of symptoms, ranging from mild discomfort to severe pain and infection. Recognizing and treating these symptoms is critical for early detection and treatment. Here are more details on the most common symptoms of pilonidal disease:
- Pain and Tenderness: Pain and tenderness in the affected area, which is typically located in the cleft of the buttocks, just above the tailbone (coccyx), is one of the primary symptoms of pilonidal disease. The pain can range from mild to severe, making sitting or engaging in certain activities difficult. Touching the area may also cause it to feel tender.
- Swelling and Redness: Swelling and redness in the affected area are common symptoms of pilonidal disease. The skin around the pilonidal cyst or sinus tracts may be inflamed and warm to the touch. The severity of the condition and the presence of infection can influence the degree of swelling and redness.
- Visible or Palpable Lump: A visible or palpable lump or mass can be felt in the affected area in many cases. This lump can be small or large, and its size can change as the cyst or sinus tracts develop. It may be accompanied by tenderness and can be distressing for the person experiencing it.
- Pus or Blood Discharge: Pilonidal disease is frequently accompanied by the discharge of pus or blood from the affected area. The cyst or sinus tracts can become infected, resulting in pus accumulation. This can lead to the formation of an abscess, which may eventually drain through a skin opening. The discharge may have an unpleasant odor and may soil undergarments.
- Foul Odor: Pilonidal disease infection can contribute to a foul odor emanating from the affected area. An unpleasant odor can be produced by the combination of bacteria, debris, and pus. Individuals with the condition may experience embarrassment and discomfort as a result of this.
- Itching or Irritation: Pilonidal disease may cause itching or irritation in the affected area. The presence of hair follicles, debris, and bacteria on the skin can cause skin irritation and persistent itching. Scratching the affected area can aggravate the symptoms and increase the likelihood of infection.
- Fever (in cases of infection): If the pilonidal cyst becomes infected, it can trigger an immune response in the body, leading to fever. Fever, along with the other symptoms listed above, may indicate an active infection that necessitates immediate medical attention.
Causes of Pilonidal Disease:
Several factors contribute to pilonidal disease development:
- Hair Follicle Abnormalities: People who have hair follicles that are abnormally positioned or shaped are more likely to develop pilonidal disease.
- Friction and Pressure: Activities that cause constant friction or pressure on the affected area, such as prolonged sitting or repetitive trauma, can contribute to the development of pilonidal disease.
- Poor Hygiene: Inadequate personal hygiene, particularly in the buttock area, can increase the risk of infection and the subsequent development of pilonidal disease.
- Excessive Sweating: Profuse sweating, especially in the buttock region, can contribute to the formation of an ideal environment for bacterial growth and infection.
- Family History: Pilonidal disease is thought to have a genetic predisposition because it occurs more frequently in people who have a family history of the condition.
Treatment Options for Pilonidal Disease:
The severity of the symptoms and the presence of infection determine the treatment for pilonidal disease. Here are some of the most commonly used treatment options:
- Conservative Management: Mild cases of pilonidal disease that are not infected may be treated conservatively. This method entails maintaining proper hygiene, such as keeping the area clean, dry, and hair-free, as well as avoiding activities that aggravate the condition.
- Incision and Drainage: When a pilonidal cyst becomes infected, a healthcare professional may need to make an incision to drain the pus and relieve pressure. This procedure is usually done with local anesthesia.
- Antibiotics: If the pilonidal cyst is infected, the underlying infection may be treated with antibiotics.
- Pilonidal Sinus Surgery: Pilonidal disease, whether recurring or chronic, frequently necessitates surgical intervention. Excision, primary closure, flap procedures, and open wound healing are among the surgical techniques available. Pilonidal sinus surgery aims to completely remove the cyst or sinus tracts, promoting healing and lowering the risk of recurrence.
- Laser and Radiowave Treatment: Laser and radiowave treatments are available at some specialized clinics to remove pilonidal sinus tracts. These techniques offer a less invasive alternative to traditional surgery, with the potential for faster healing and less scarring.
Pilonidal Sinus Surgery
Pilonidal sinus surgery is a common procedure used to treat recurrent or chronic pilonidal disease. The goal of surgery is to completely remove the cyst or sinus tracts, promote healing, and lower the risk of recurrence. There are several surgical techniques available, and the procedure chosen is determined by a number of factors, including the severity of the condition, the presence of infection, and the patient’s overall health.
- Excision and Primary Closure: Excision and primary closure are two traditional surgical techniques. The surgeon removes the entire pilonidal cyst, sinus tracts, and any infected tissue during this procedure. Sutures are then used to close the wound, allowing for primary healing. This technique is appropriate for small or early-stage pilonidal disease and has a shorter recovery time than other surgical approaches. It may not, however, be appropriate for larger or more complex cases.
- Flap Procedures: Flap procedures are commonly used to treat more severe or recurring pilonidal disease. These methods entail using nearby healthy tissue to reconstruct the wound and promote healing. The Limberg flap, for example, involves the surgeon creating a triangular-shaped flap of skin adjacent to the wound and rotating it to cover the surgical site. Flap procedures improve wound closure, reduce incision tension, and promote healing. They are especially useful in complex cases or when primary closure is not possible.
- Open Wound Healing: When the pilonidal disease is extensive or there are multiple sinus tracts, the surgeon may choose open wound healing. The wound is left open and allowed to heal gradually from the bottom up in this method. The wound is dressed on a regular basis, and the healing process can take several weeks to months. Although it necessitates more extensive wound care and a longer recovery period, open wound healing has been shown to be effective in preventing recurrence by encouraging granulation and wound closure from the inside out.
- Laser and Radiowave Treatment: In recent years, minimally invasive techniques such as laser and radiowave treatment have gained popularity for the treatment of pilonidal disease. These methods use lasers or radiowaves to vaporize and remove the sinus tracts while sparing the surrounding healthy tissue. When compared to traditional surgery, they are associated with less post-operative pain, less scarring, and shorter recovery times. These procedures, however, may not be appropriate for all cases and are often best suited for early-stage or uncomplicated pilonidal disease.
Recovery and Prevention: Proper post-operative care is essential following pilonidal sinus surgery or any other treatment. It may include wound care, regular dressing changes, and, if necessary, antibiotics. Preventive measures, such as maintaining good personal hygiene, avoiding prolonged sitting, and keeping the area clean and dry, are also important to reduce the risk of recurrence.
Contact the Experts Today!
The specialists at Pilonidal Experts can help you take control of your pilonidal disease journey. Our specialized knowledge, customized treatments, and cutting-edge options can help alleviate symptoms and prevent recurrences. Don’t go through it alone; reach out to us today for compassionate care and support. Pilonidal Experts can help you regain your health.